But bioidentical progesterone supplementation can help alleviate digestive issues and naturally boost gut health in multiple ways.
The Gut-Brain-Hormone Connection
The gut is often described as the body's "second brain" — and for good reason. It contains over 100 million nerve cells and produces around 95% of the body's serotonin, a neurotransmitter that regulates mood, sleep, and appetite. This extensive network, known as the enteric nervous system, communicates constantly with the brain via the vagus nerve.
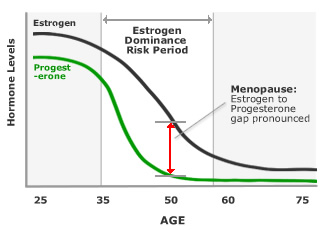
Hormones play a crucial role in this communication. Progesterone, oestrogen, and cortisol all influence how the gut functions, how quickly food moves through the digestive tract, and how the body responds to inflammation. When progesterone levels decline during perimenopause and menopause, this finely tuned system can be thrown off balance.
This is why so many women in their 40s and 50s experience digestive problems they have never had before — bloating, constipation, acid reflux, food sensitivities, and irritable bowel symptoms that seem to appear out of nowhere. Understanding the connection between hormonal changes and gut health is the first step towards finding relief.
Common Digestive Symptoms During Menopause
Many women are surprised to discover that their digestive complaints are linked to menopause. While hot flushes and night sweats are well-known menopause symptoms, gut-related issues are frequently overlooked. Common digestive symptoms during menopause include:
- Bloating and abdominal distension, particularly after meals
- Constipation or changes in bowel habits
- Increased sensitivity to certain foods
- Acid reflux or heartburn
- IBS-like symptoms (alternating constipation and diarrhoea)
- Nausea
- Excessive gas and flatulence
These symptoms often coincide with other hormonal changes and may be compounded by the weight gain and stress that commonly accompany the menopause transition. Addressing the underlying hormonal imbalance — particularly the drop in progesterone — can help resolve many of these digestive complaints.
Gut Motility Regulation
Progesterone affects the enteric nervous system, which controls gastrointestinal motility. It modulates smooth muscle activity in the gut through binding to progesterone receptors on the smooth muscle cells of the intestines.
This interaction influences the release of neurotransmitters that either stimulate or inhibit muscle contractions, thus helping to maintain regular bowel movements and preventing constipation.
Studies have shown that progesterone can enhance gastric emptying and transit time in the intestines, which can be beneficial for menopausal women experiencing slowed gastrointestinal motility.
When progesterone levels fall during menopause, the smooth muscle of the gut can become sluggish, leading to slower transit times and the uncomfortable bloating and constipation that many women report. This is a direct consequence of hormonal change rather than dietary factors alone, which is why dietary modifications without hormonal support may provide only partial relief.
Anti-inflammatory Action
Progesterone exhibits anti-inflammatory effects by inhibiting the release of pro-inflammatory cytokines and reducing the infiltration of inflammatory cells into the gut mucosa.
It acts on the nuclear factor kappa B (NF-κB) pathway, a key regulator of inflammation, thereby downregulating the expression of genes involved in the inflammatory response.
This anti-inflammatory effect can help alleviate symptoms of inflammatory bowel diseases (IBD) and IBS, which can be exacerbated by hormonal changes during menopause.
Chronic low-grade inflammation in the gut is increasingly recognised as a driver of many digestive complaints. As progesterone's natural anti-inflammatory action diminishes during menopause, the gut becomes more vulnerable to inflammatory responses. This can create a cycle where inflammation impairs digestion, which in turn increases stress on the gut lining, leading to further inflammation. Supplementing with bioidentical progesterone may help to break this cycle by restoring the hormone's protective anti-inflammatory effects.
Modulation of Gut Microbiome
Progesterone has been shown to influence the composition and diversity of the gut microbiome. It promotes the growth of beneficial bacteria, such as Lactobacillus and Bifidobacterium, which play a crucial role in maintaining gut health.
The hormone can alter the gut environment by affecting the production of mucus and antimicrobial peptides, creating conditions that favour the growth of beneficial microbes while inhibiting pathogenic bacteria.
A balanced microbiome is essential for effective digestion, nutrient absorption, and immune function.
Research has shown that the gut microbiome itself plays a role in hormone metabolism through what is known as the "estrobolome" — the collection of gut bacteria that metabolise oestrogens. A disrupted microbiome can interfere with hormone processing, potentially worsening oestrogen dominance. This creates a two-way relationship: hormonal changes affect the microbiome, and in turn, a disrupted microbiome can exacerbate hormonal imbalances. Supporting both progesterone levels and the microbiome simultaneously is therefore an important strategy during menopause.
Enhanced Nutrient Absorption
Progesterone's role in maintaining the integrity of the gut lining is crucial for optimal nutrient absorption.
It supports the tight junctions between intestinal epithelial cells, preventing increased intestinal permeability (leaky gut syndrome), which can lead to malabsorption of nutrients.
By preserving the gut barrier function, progesterone ensures that essential nutrients are efficiently absorbed into the bloodstream, which is vital for menopausal women who require adequate nutrition to support overall health and well-being.
This is particularly important during menopause because the body's need for certain nutrients increases. Calcium and vitamin D absorption is critical for maintaining bone density and reducing the risk of osteoporosis. Magnesium — essential for sleep, mood, and muscle function — can also be poorly absorbed when gut integrity is compromised. By supporting the gut lining, progesterone helps ensure that the nutrients from food and supplements are actually reaching the body's cells where they are needed.
The Stress-Gut Connection During Menopause
Menopause frequently coincides with a period of heightened stress — whether from physical symptoms, sleep disruption, life changes, or the hormonal shifts themselves. Stress has a profound effect on gut health. When the body is under stress, cortisol levels rise, which can slow digestion, increase gut permeability, reduce blood flow to the digestive organs, and alter the microbiome.
Progesterone has a natural calming effect on the nervous system. It is a precursor to allopregnanolone, a neurosteroid that acts on GABA receptors in the brain — the same receptors targeted by anti-anxiety medications. When progesterone declines during menopause, this calming effect is reduced, potentially increasing anxiety and stress levels. The resulting rise in cortisol can then directly impair gut function, creating a vicious cycle of stress, poor digestion, and further hormonal disruption.
Addressing progesterone decline may therefore benefit gut health not only through the direct mechanisms described above, but also indirectly by helping to manage the stress response during this challenging transition. As always, speak to your healthcare professional for personalised advice.
Practical Dietary Tips for Gut Health During Menopause
While hormonal support is important, dietary and lifestyle choices can also make a significant difference to gut health during menopause. Consider the following:
- Eat plenty of fibre: Vegetables, fruits, whole grains, and legumes feed beneficial gut bacteria and support regular bowel movements. Aim for a wide variety of plant foods — diversity in your diet supports diversity in your microbiome.
- Include fermented foods: Natural yoghurt, kefir, sauerkraut, kimchi, and kombucha provide live beneficial bacteria that can help replenish the gut microbiome.
- Eat prebiotic-rich foods: Garlic, onions, leeks, asparagus, and bananas contain prebiotic fibres that feed the beneficial bacteria already present in your gut.
- Stay hydrated: Adequate water intake is essential for digestive health and helps prevent constipation.
- Reduce processed foods and sugar: These can feed pathogenic bacteria and contribute to gut inflammation.
- Consider omega-3 fatty acids: Found in oily fish, flaxseeds, and walnuts, omega-3s have anti-inflammatory properties that can support gut health.
- Manage stress: Practices such as walking, yoga, deep breathing, and adequate sleep all support both gut health and hormonal balance during menopause.
Supporting Your Gut Health with Wellsprings
If you are experiencing digestive symptoms during menopause, addressing the underlying hormonal imbalance may be an important part of finding relief. Wellsprings Serenity provides USP-grade natural progesterone in a liposomal cream formulation designed for optimal transdermal absorption.
For women who also need oestrogen support, Wellsprings 20-1 combines natural progesterone with a small amount of natural oestrogen. And Wellsprings Menopause Capsules — containing turmeric, ashwagandha, and other carefully selected ingredients — may provide additional support for overall wellbeing during the menopause transition.
Gut health is deeply intertwined with hormonal health, and understanding this connection is key to managing menopause symptoms effectively. We always recommend speaking to your healthcare professional to discuss the best approach for your individual circumstances.
References
- Lee, J.R. (1996). What Your Doctor May Not Tell You About Menopause. Warner Books.
- Rushton, A. & Bond, Dr S. Natural Progesterone. Wellsprings Health.
- Baker, J.M., Al-Nakkash, L. & Herbst-Kralovetz, M.M. (2017). Estrogen–gut microbiome axis: Physiological and clinical implications. Maturitas, 103, 45–53.
- Mulak, A. et al. (2014). Sex hormones in the modulation of irritable bowel syndrome. World Journal of Gastroenterology, 20(10), 2433–2448.
Medical Disclaimer
This article is for general informational purposes only and is not intended as medical advice. It should not be used to diagnose or treat any health condition. Always consult your doctor or qualified healthcare professional before starting any new treatment or making changes to your existing care. Every woman is unique and individual results may vary.
This article is for general informational purposes only and is not intended as medical advice. It should not be used to diagnose or treat any health condition. Always consult your doctor or qualified healthcare professional before starting any new treatment or making changes to your existing care. Every woman is unique and individual results may vary.
Menopause and Hot Flushes
Doctors and Natural Progesterone
Find out what causes this common symptom, and how to get relief
Progesterone supplementation can naturally boost gut health
Hear what doctors have to say about natural progesterone and its benefits
Natural progesterone can be an effective treatment for this serious condition
What happens to hormones at menopause and how can symptoms be treated?
Understand what's behind the increased incidence of oestrogen dominance in the western world
How can a cream deliver progesterone into the body?
What are bioidentical hormones and why are they relevant to your health
Learn how to get the most from your Wellsprings bioidentical hormone creams
Wellsprings offers two varieties of natural progesterone cream. Read on to find out which is best for you
Oestrogen dominance can interfere with thyroid hormone activity
Despite claims to the contrary, Yam Extract does NOT contain progesterone or raise progesterone levels in the body
All information given on this site is for general interest only. Every woman is unique. Your results may vary.