In the Western world, more women die of complications related to hip fractures than from cancer. Osteoporosis is believed to be the cause of millions of bone fractures per year worldwide. Yet despite its severity, it is a condition that can be addressed — and natural progesterone may play an important role.
What is osteoporosis?
Osteoporosis literally means ‘porous bones’. It is a condition where the internal structure of bones deteriorates, becoming thin, weak, and prone to fracture. Even a minor fall, bump, or sudden movement can result in a broken bone.
The most common fracture sites are the hip, spine, and wrist, though osteoporosis affects the entire skeleton. Spinal fractures can occur without any impact at all, causing the vertebrae to gradually compress and leading to loss of height and the stooped posture sometimes seen in older women.
Osteoporosis can be preceded by a condition called osteopenia, in which bone density starts to decrease below normal levels but has not yet reached the threshold for an osteoporosis diagnosis. Osteopenia is a warning sign — if left unaddressed, it can progress to full osteoporosis.
Why does bone density decline during menopause?
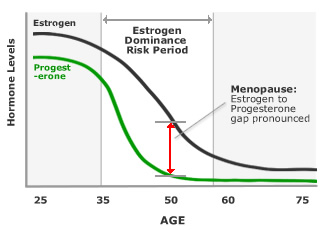
It is widely believed that modern lifestyles and eating habits, combined with environmental pollutants, are largely to blame for a general decline in bone quality amongst mature Western adults. The hormonal changes of menopause then further accelerate the problem.
To understand why, it helps to know how bones work. Bone is not a static structure — it is living tissue that is constantly being remodelled through two processes:
- Osteoclasts — cells that break down and remove old or damaged bone tissue
- Osteoblasts — cells that build new bone tissue to replace it
In a healthy skeleton, these two processes are balanced. Old bone is removed and new bone is built at roughly the same rate.
Both oestrogen and progesterone play crucial roles in this process, but their roles are different:
- Oestrogen primarily slows the osteoclasts — it reduces the rate of bone breakdown
- Progesterone stimulates the osteoblasts — it promotes the formation of new bone
During menopause, both hormones decline. The loss of oestrogen means bone is broken down faster, while the loss of progesterone means less new bone is being built to replace it. This double effect can lead to rapid bone density loss — studies suggest women can lose up to 20% of their bone density in the 5 to 7 years following menopause.
This is why the menopausal years are the most critical time for bone health, and why addressing progesterone deficiency — not just oestrogen — is so important.
The overlooked role of progesterone in bone health
Most conventional approaches to osteoporosis focus on oestrogen and calcium. While both are important, they primarily address one side of the equation — slowing bone loss. Progesterone’s role in actually building new bone has been largely overlooked by mainstream medicine.
Dr John R. Lee, who spent over 20 years prescribing and studying natural progesterone, dedicated much of that time to researching its effectiveness in treating osteoporosis. His work provided compelling evidence for progesterone’s bone-building properties.
In his clinical studies, Dr Lee documented a significant increase in bone mineral density amongst post-menopausal women using transdermal progesterone cream over a three-year period. This contrasts sharply with the average drop in bone density experienced by women taking no treatment at all.
His research suggested that natural progesterone supplementation could not only halt the decline of bone mass but actually reverse it, strengthening bones and protecting women against fractures in later life.
As Dr Lee wrote: “Post-menopausal osteoporosis is a disease of inadequate osteoblast-mediated new bone formation secondary to progesterone deficiency. Progesterone restores osteoblast function. Natural progesterone hormone is an essential factor in the proper treatment of osteoporosis.”
Since bone mass depletion accelerates rapidly during menopause, natural progesterone supplementation at this time can offer a double benefit — relieving menopausal symptoms while simultaneously supporting bone health.
Natural progesterone vs conventional osteoporosis treatments
The most commonly prescribed drugs for osteoporosis are bisphosphonates (such as alendronate and risedronate). These work by slowing the osteoclasts — reducing the rate at which old bone is broken down.
While bisphosphonates can slow bone loss, they come with significant concerns:
- They can cause gastrointestinal problems, including nausea and oesophageal irritation
- Long-term use has been linked to an increased risk of atypical femoral fractures — unusual breaks in the thigh bone
- A rare but serious side effect called osteonecrosis of the jaw (deterioration of the jawbone) has been reported
- Because they slow the removal of old bone, the bone that remains may become older and more brittle over time, even though density measurements look improved
Natural progesterone, being bioidentical to the body’s own hormone, has no such side effects. Rather than simply slowing the breakdown of old bone, it addresses the other side of the equation — promoting the formation of new, healthy bone tissue.
This does not mean that bisphosphonates or other treatments are never appropriate — your healthcare professional is best placed to advise on the right approach for your individual situation. However, progesterone supplementation offers a complementary or alternative approach that many women and their healthcare providers find valuable.
Risk factors for osteoporosis
Some women are at higher risk of developing osteoporosis. Being aware of your risk factors can help you take preventive action:
- Age and menopause: The years during and after menopause are the highest-risk period due to rapid hormonal decline
- Family history: A parent or sibling with osteoporosis or a history of hip fracture increases your risk
- Body frame: Women with smaller, thinner frames tend to have less bone mass to start with
- Early menopause: Women who experience menopause before age 45 have a longer period of reduced hormone levels
- Low calcium and vitamin D intake: Both are essential for bone health throughout life
- Sedentary lifestyle: Weight-bearing exercise is vital for maintaining bone density
- Smoking: Cigarette smoking is associated with increased bone loss
- Excessive alcohol: More than two drinks per day has been linked to reduced bone density
- Certain medications: Long-term use of corticosteroids and some other drugs can reduce bone density
Protecting your bones — a practical approach
A comprehensive approach to bone health during menopause combines hormonal support with lifestyle measures:
Address the hormonal imbalance
Supplementing with Wellsprings Serenity can help restore progesterone levels, supporting the osteoblasts that build new bone. For women who are also oestrogen-deficient, a combination cream like Wellsprings 20-1 addresses both hormones.
Weight-bearing and resistance exercise
Exercise that loads the skeleton stimulates bone formation. Walking, jogging, dancing, stair climbing, and resistance training (weights, resistance bands) are all effective. Aim for regular activity — consistency matters more than intensity.
Calcium and vitamin D
Calcium is the primary mineral in bone, and vitamin D is essential for calcium absorption. Good dietary sources of calcium include dairy products, leafy greens, sardines, and fortified foods. Vitamin D is produced by the skin in response to sunlight, but supplementation may be needed, particularly in northern climates or during winter.
Reduce risk factors you can control
Stop smoking, moderate alcohol intake, and review any medications that may affect bone density with your healthcare professional. Maintaining a healthy weight is also important — being underweight is a risk factor for osteoporosis.
Get a bone density scan
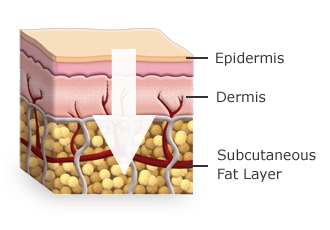
If you are post-menopausal or have risk factors, ask your healthcare professional about a DEXA scan (dual-energy X-ray absorptiometry). This painless test measures your bone mineral density and can detect osteopenia or osteoporosis before a fracture occurs.
Getting started
Wellsprings Serenity is a premium natural progesterone cream that has been helping women overcome symptoms of hormone imbalance, including osteoporosis, since 1997. For guidance on how to use it, see our guide to using Wellsprings creams.
Learn more about natural progesterone and its properties, or read the stories of women who have found relief from menopause symptoms.
References
- Lee, J.R. (1993). Natural Progesterone: The Multiple Roles of a Remarkable Hormone. BLL Publishing.
- Prior, J.C. Progesterone as a bone-trophic hormone. Endocrine Reviews.
- Rushton, A. & Bond, Dr S. Natural Progesterone. Wellsprings Health.
Medical Disclaimer
This article is for general informational purposes only and is not intended as medical advice. It should not be used to diagnose or treat any health condition. Always consult your doctor or qualified healthcare professional before starting any new treatment or making changes to your existing care. Every woman is unique and individual results may vary.
This article is for general informational purposes only and is not intended as medical advice. It should not be used to diagnose or treat any health condition. Always consult your doctor or qualified healthcare professional before starting any new treatment or making changes to your existing care. Every woman is unique and individual results may vary.
Natural Progesterone
Menopause Symptoms and the Role of Ho...
Find out what causes this common symptom, and how to get relief
Progesterone supplementation can naturally boost gut health
Hear what doctors have to say about natural progesterone and its benefits
Natural progesterone can be an effective treatment for this serious condition
What happens to hormones at menopause and how can symptoms be treated?
Understand what's behind the increased incidence of oestrogen dominance in the western world
How can a cream deliver progesterone into the body?
What are bioidentical hormones and why are they relevant to your health
Learn how to get the most from your Wellsprings bioidentical hormone creams with proper application techniques, timing, and usage guidelines
Wellsprings offers two varieties of natural progesterone cream. Read on to find out which is best for you
Oestrogen dominance can interfere with thyroid hormone activity
Despite claims to the contrary, Yam Extract does NOT contain progesterone or raise progesterone levels in the body
All information given on this site is for general interest only. Every woman is unique. Your results may vary.